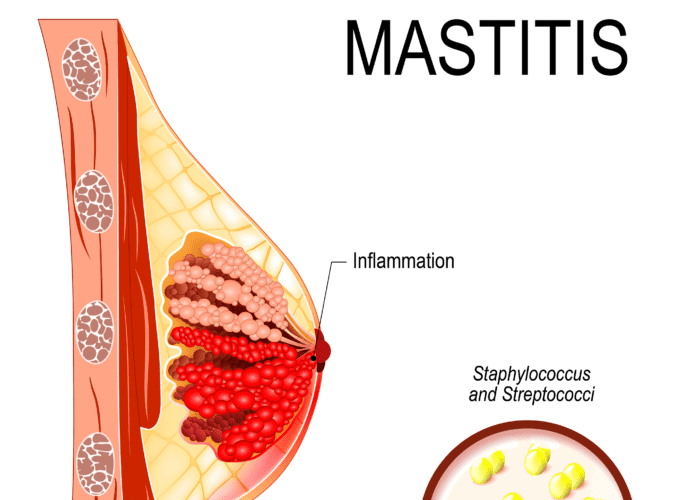
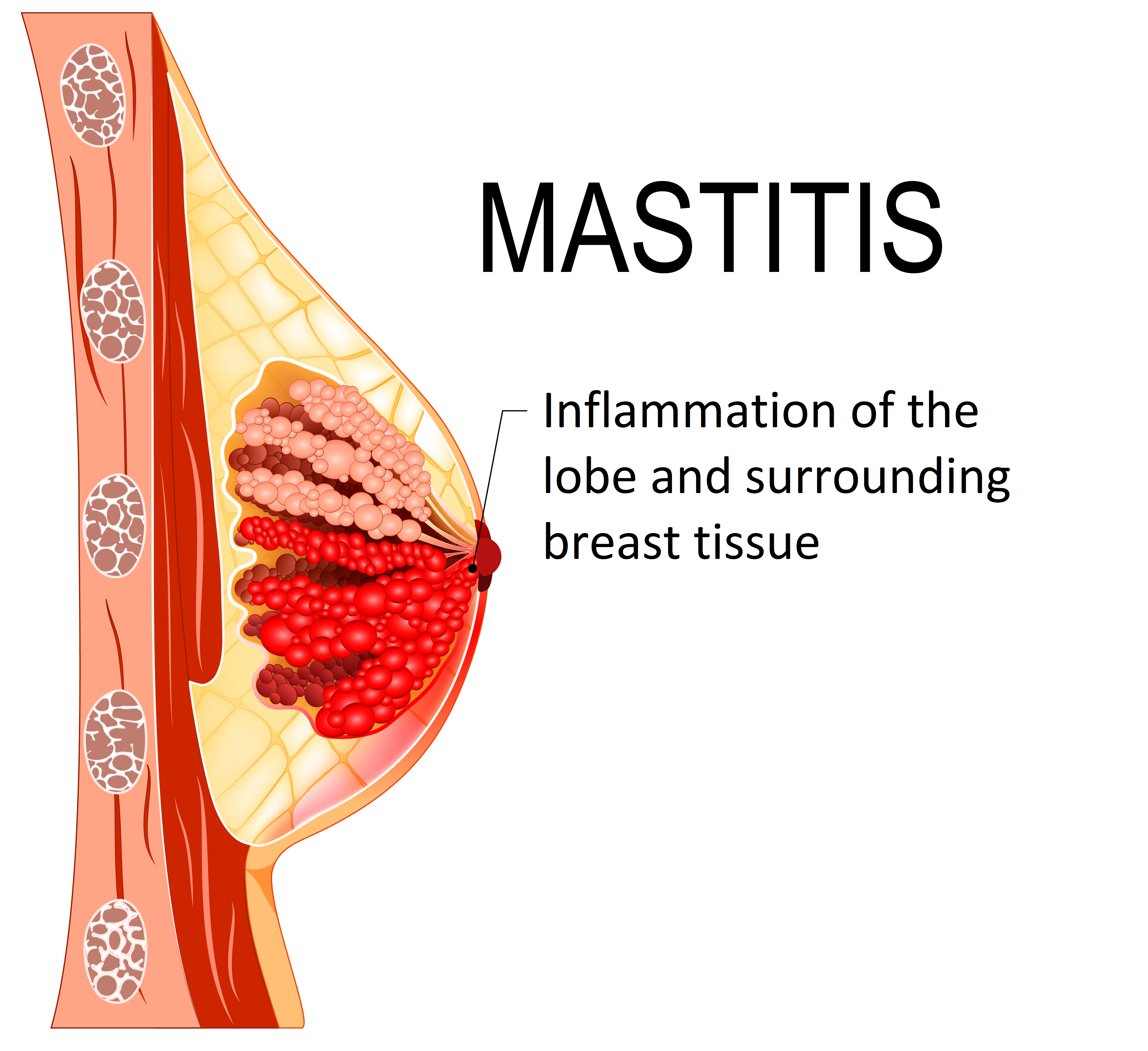
If you google mastitis, it’s more than likely all the content coming up for you is to do with breastfeeding parents. While mastitis most commonly occurs in breastfeeding women, that’s not the only time you can get it! Women also aren’t the only ones who can get mastitis, with a small percentage of men also finding themselves with a mastitis condition.
When mastitis occurs in someone who is not lactating it’s called non-lactational mastitis. Like lactational mastitis, most people who get non-lactational mastitis are usually women of reproductive age.
Mastitis can happen when bacteria is introduced to the breast tissue. In lactating people, this might be if you have nipple trauma from feeding bub. In the non-lactating person, it might come in the form of a graze or cut on the skin, an infected piercing, or even eczema that has become infected. What all the above have in common is they are an open channel from the outside world to your breast tissue enabling bacteria to get in.
Unfortunately, when we have diabetes and other conditions that weaken our immune system, we’re left susceptible to a host of infections. The breast tissue is just like any part of the body, in can get infected as much as the next part. If we have conditions that affect and lower our immune system, it means that when bacteria are introduced to the tissue, the body has a tougher time fighting it off. This means that what might not have been a problem for someone with a healthy immune system, can end up a problem for you! Similarly to how we can have internal issues that cause a weakened immune system, outside factors like radiation therapy and
This type of mastitis occurs in the milk ducts of the breast tissue. What happens is the milk ducts enlarge and thicken which causes a blockage. This blockage then triggers an inflammation process – if you’re familiar with lactational mastitis you’ll notice the similarities in how it happens!
GM is a chronic inflammatory breast condition; it can be a very distressing and painful condition to develop. GM is not actually mastitis, it’s a different condition but it can mimic the symptoms of mastitis making it hard to find out what is actually going on. It also tends to happen in the same group of people as non-lactational mastitis affecting mostly women of reproductive age. A few things that make the risk of GM higher include current or previous pregnancy and the oral contraceptive pill.
While the most common people to experience non-lactating mastitis are adults, they are not the only group of people that can be affected. Rarely, newborns in their first 8 weeks of life may develop mastitis. They will have red, painful breast tissue that sometimes produces discharge. Older children may develop what is called thelitis, which is when there is an inflammation of the nipple.
You have a breast lump and inflammation, is there a cause for concern about cancer? As health professionals, it’s always something our practitioners have in the backs of our mind. Unfortunately, there is overlap of symptoms, but we’re also looking for other symptoms that indicate a serious concern too. Not only are we looking for what you’ve noticed going on, when a health professional assesses you, we’re looking for differences in the way a lump feels and presents. If you are ever concerned about a breast lump, the best thing you can do for yourself is get it checked by a health professional.
It’s important to consider that like lactational mastitis, one of the main things we’re dealing with is inflammation. What happens when we have inflammation and infections is the release of a protein called cytokines. This triggers the body’s immune cells which take care of the problem. These immune cells arrive and hang around, and then you get the red, hot, angry breast tissue. What we want to do is address this inflammation. We can use techniques like hot or cold compresses, anti-inflammatory medications (always consult your doctor or pharmacist before taking new medication), and we can even use hands-on techniques.
In using hands-on techniques, our goal is to encourage that inflammatory fluid to leave the breast tissue. We are also encouraging blood flow which brings new immune cells, nutrients, and oxygen to the area which are all important for healing. At MMC we also like to look at the bigger picture, not just the breast alone. We consider what other aspects of your body may be restricted causing blockages in fluid flow and pain.
When you have non-lactational mastitis, it might seem like there isn’t much help out there – particularly when most information is geared towards breastfeeding mothers. The good news is, you can still see a few health professionals to get help with your condition. Your family doctor is always a great place to go, they can help to manage infections with medications and advice. Melbourne Mastitis Clinic is also a resource you can use! We’ll talk through what is going on for you and treat the breast tissue that is inflamed and sore. We have in person consultations as well as virtual which are great for those of you that don’t live in Melbourne! You can find our online bookings page HERE or call us on 9859 5059 to book or if you have questions!
Sources
AbdelHadi, M., & Bukharie, H. A. (2005). Breast infections in non-lactating women. Journal of Family and Community Medicine, 12(3), 133-137.
Tan, H., Li, R., Peng, W., Liu, H., Gu, Y., & Shen, X. Radiological and clinical features of adult non-puerperal mastitis. (2013). British Journal of Radiology, 86(1024).
Brennan, M. E., Morgan, M., Heilat, G. B., & Kanesalingam, K. (2020). Granulomatous lobular mastitis: Clinical update and case study. Australian Journal of General Practice, 49(1-2).
Boakes, E., Woods, A., Johnson, N., & Kadoglou, N. (2018). Breast Infection: A review of Diagnosis and Management Practices. European Journal of Breast Health, 14(3), 136-143.
Fill in the contact form below and we will reply ASAP.
